Behind the Needle: Why Scotland Is Finally Regulating Non-Surgical Cosmetic Procedures
By Abby Paterson
The UK non-surgical cosmetic industry was valued at around £3.6 billion. So why did it take so long for proper regulation to be introduced into this billion-pound industry? The use of Botox and dermal fillers has become increasingly normalised within the beauty industry. It’s not uncommon to get Botox on a lunch break or get offered lip filler at your local nail salon. But how well do we really know the people behind the needle?
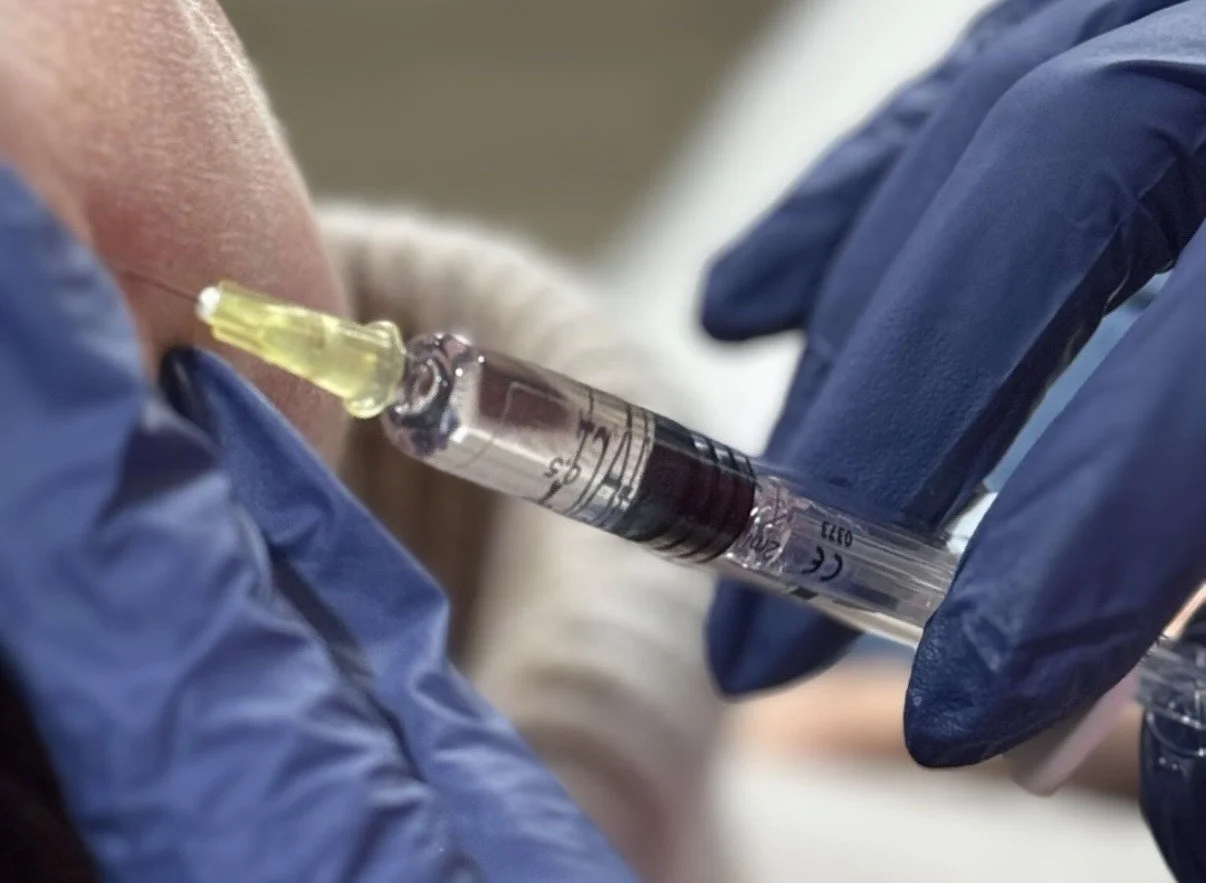
Non-surgical cosmetic injection, admistered by Dr Meera Singh
Research from the University College London found that 68% of injectors in the UK are not doctors, and with around 900,000 Botox injections being carried out across the UK every year, it’s clear this industry is only expanding. These figures only amplify concerns around training standards; patient safety and the growing number of procedures performed outside healthcare environments.
Andrew Rankin, Trustee and Co-Chair at the Joint Council for Cosmetic Practitioners (JCCP), said: “The problem is not how quickly the sector has expanded. It’s how slow the regulation has been to keep up with it.”
While social media tries to market cosmetic injections as the next quick-fix beauty treatments, they undermine the real medical risk involved. The British Association of Aesthetic Plastic Surgeons repeatedly warned that poorly regulated treatments could lead to serious physical and psychological harm.
Filler is one of the most common types of minimally invasive treatments. If administered incorrectly it can lead to serious complications, such as infection, vascular occlusion, tissue damage, and in rare cases blindness. Despite these risks, a Scottish Parliament research briefing found that these procedures were routinely being carried out in beauty salons and private homes.
Dr Meera Singh preparing to inject a client during a cosmetic procedure.
Dr Meera Singh, an NHS GP, and cosmetic injector said: “Whenever I say to someone, ‘What did your previous practitioner use?’ They never know, they don’t know whether they had filler, sometimes they don’t know if they had Botox.”
Unregulated clinics lead to uninformed patients. If the injector doesn’t know what they’re providing neither will the patient and this becomes even more complex when it comes to treating complications from cosmetic injections.
In a freedom of information response, the Scottish Government acknowledged that the non-surgical cosmetics sector had been “largely unregulated” and admitted NHS systems do not consistently record complications linked to cosmetic procedures, making the true scale of harm difficult to measure.
Rankin said: “The concerns for safety were largely anecdotal and, in some instances, theoretical. But over time… evidence of the risks has grown.”
This hesitance to actively address the issue is reflected in the lack of data around cosmetic complications in Scotland. The blind spot created by the gap in regulation means cases often surface through GPs, emergency departments, or private healthcare, without being formally tracked as part of a wider public health picture.
Although information from Save Face, a UK Government approved register of accredited practitioners, provides some insight. The company received almost 3,000 complaints in 2022, with over two-thirds of those complaints relating to dermal fillers and almost a quarter relating to Botox.
For Dr Singh, those complications are visible in her day-to-day practice.
She said: “I have patients or clients who have come to me either with a history of having had a complication or with a complication. Sometimes those people they’ve gone to have blocked them and not had any contact details and not been able to have any of the complication resolved.”
Her experience exposes the harsh reality about accountability within the aesthetics industry. Within these unregulated spaces, there’s no specific authority to hold people practising aesthetics illegally or unsafely responsible. This lack of oversight is likely what’s contributed to non-medical aestheticians doubling from 12% to 24.8% according to The National Library of Medicine.
Rankin said: “It’s acting responsibly and transparently and being accountable for that practice that I would say is critically important.”
On 17 March 2026, The Non-surgical Procedures and Functions of Medical Reviewers (Scotland) Bill was passed by the Scottish Parliament, making Scotland the first UK nation to pass this level of formal regulation on non-surgical cosmetics.
The Bill would see higher-risk procedures including Botox and fillers to be supervised by healthcare professionals and carried out in premises regulated by Healthcare Improvement Scotland. It also makes it illegal to provide non-surgical cosmetic procedures to anyone under the age of 18, with penalties of up to £20,000 for those who violate the legislation.
Healthcare Improvement Scotland will oversee this new system, bringing parts of the aesthetics industry closer to healthcare-style regulation through stricter standards on safety, premises, and practitioner oversight. The Scottish Government said businesses will have until at least September 2027 to meet the new licensing requirements as the rules are phased in.
Aesthetic injector Nurse Leah also discussed the proposed regulations on social media, reflecting wider industry discussion around how the new rules may affect practitioners.
Nurse Leah speaking about Scotland’s new regulations for non-surgical cosmetic procedures.
While many practitioners support stronger regulation, questions remain over how some parts of the legislation will work in practice.
Dr Singh said: “I think having more regulations for all practitioners is good, but some aren’t necessarily realistic, such as having a prescriber there the whole time during appointments.”
Training standards also remain a major concern across the industry. While some practitioners undertake extensive medical and clinical education, others enter aesthetics through short courses with little consistency between providers.
Dr Singh said: “I feel like some of the training that’s offered as well is not consistent amongst all academies or trainers, but yeah complications issues are definitely still a problem.”
Supporters of Scotland’s new regulations argue the legislation is ultimately about bringing accountability to an industry that evolved faster than the systems designed to regulate it.
Rankin said: “The one thing that I would say is that it will be absolutely clear what is safe and legal practice in the future.”
Scotland took too long to implement regulation but, now appears to be leading the way as the first UK nation to take a clear legal stance on unregulated cosmetic procedures. Whether that intervention proves transformative or simply corrective will depend on how far and how fast the new regulations can reshape an industry that has already defined its own rules.